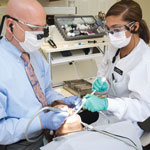
Ergonomics Helps Dentists Reach Their Potential.
“Go buy 12 white shirts and 12 new silk ties.” As a new dentist seeking to grow my practice, I called Dr. Dick Barnes in the 1990s and I’ll never forget his advice. It was not what I expected. After a moment, Dr. Barnes repeated himself: “Go buy 12 white shirts and 12 new silk ties.”
I hired Dr. Barnes as a consultant because even though I knew I was a great dentist, I didn’t believe that my level of success reflected my skills. I expected him to tell me to do something about my dentistry. Instead, after I gave him a list of excuses for why I wasn’t as successful as I thought I should be, Dr. Barnes looked across the table at me and told me to change my wardrobe.
I was not entirely convinced that his advice was the answer to my dilemma so I only partially bought into his suggestion. I purchased half a dozen shirts and half a dozen ties—in other words, half a commitment. Even though I was skeptical, when a guru tells you to do something, you do it!
Wearing my new clothes, I then did what Dr. Barnes suggested and presented comprehensive dentistry. Here’s what happened: I became a better dentist and was wildly successful.
In fact, I couldn’t physically deliver all the treatments for my patients. After a few years of high production, I wound up in physical pain. I was at the limits of the amount of dentistry that I could get done in the way I was doing it.
In the 1990s, I had asked Dr. Barnes to help “fix” my practice. After following his advice, I had so much success that I found myself seeking the advice of physicians about how to fix myself physically. Several physicians advised me to consider quitting dentistry because my health was reaching a breaking point.
Luckily, I didn’t listen to them. The search for an answer to my health problems signaled the beginning of a study of health and performance that has lasted for more than two decades. From my studies, two significant things happened: first, I became healthy. Second, I became even more productive in my dental practice. It was a win-win situation.
When other dentists discovered my practice’s success, they began to ask me for assistance. Most of them weren’t experiencing the physical problems that I was, but many faced serious productivity and financial roadblocks. Originally, my goal in dentistry was to survive and feed my family. I didn’t plan to start an additional company that would become the largest independent designer of dental offices in the country. But that’s just what happened.
My company, Design Ergonomics, and its sister company, Ergonomic Products, offer industry-leading design services and high-performance dental delivery systems. Our goal is to help dentists achieve higher production with ergonomic solutions—design plans, clinical training, and office setups and equipment.
What is Ergonomics?
Ergonomics is the study of how people interface with machines and the application of improvements to address issues of health, safety, and efficiency. In other words, it’s about making the most of how people work in their environment. Design Ergonomics develops equipment and offices to maximize productivity and comfort for practitioners and patients alike.
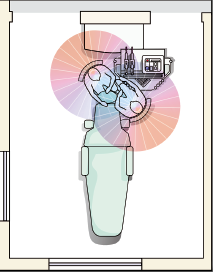
Dentists typically have a few misconceptions about using their instruments efficiently. First, dentists tend to think that handpiece placement is very important. Ultimately, however, handpiece use accounts for only about 7 to 10 percent of treatment time—a relatively small amount of the treatment time required for a productive dental practitioner.
Therefore, doctors have more flexibility with handpiece placement than they suppose. In other words, handpieces don’t need to be placed right in the patient’s face for maximum efficiency, because it is the worst place to locate them from a case-acceptance standpoint.
Trying to get patients to buy dentistry while they are forced to stare at terrifying devices is usually a bad idea.
A second misconception is that loupe focal length should be as long as possible. Declination angle is much more important to good ergonomic positioning than focal length. Fixating on extreme focal length creates many other problems. Most significantly, it displaces the dental assistant out and away from the operatory field.
The third misconception has to do with the use of belly bars for assistants. If your assistants depend on belly bars, it means your positioning is all wrong. When the doctor has the patient in the wrong position, the assistant is forced to hang over a “hook” (the belly bar), so as not to fall into the patient’s lap. If an office depends on belly bars, it means the overall patient position needs to change.
![]()
Making Ergonomics Work
A dental office should be a beautiful and comfortable place, but it has to function properly for the dental team members, too. A lot of dental offices are poorly designed so doctors have obstacles to production. Such obstacles can be fixed. Often, dental practices can flow better without making any major changes. Simple changes of instrumentation can help speed up production.
When considering ergonomic changes at a dental office, start at a macroscopic level. In general, dentists tend to engage on the microscopic level—they want to know which gadget will solve a particular problem.
In contrast, start at the level of the overall flow of the practice—look at how everything functions together. Don’t look at one particular problem or issue. It’s always good to think about the practice on a bigger scale. For example, analyze how you get a room ready for the next patient. A typical office takes 10 to 15 minutes to reset a room for the next patient. The rate-limiting step is the time it takes for the disinfectant to work, which is four minutes. Therefore, it should actually take just four minutes to turn a room around.
Analyze your practice and see how long it takes your team to reset a treatment room. Devise ways to shorten this frequent, predictable process, and it will free up time for other appointments.
The size of the dental practice doesn’t make a difference in the ability to improve the overall flow; the principles of flow are the same. However, a 3-chair office is different than a 15-chair office, and each requires distinct modifications.
Dental schools don’t teach the optimal way to set up an office, especially at a larger practice. And most doctors don’t understand how to scale up. At a certain point, a doctor may get extra associates in a five-chair office, and often they bump into each other until they realize, “This doesn’t work.”
I worked with a practice in Reno, NV, called Sala Family Dental. In this practice, Dr. Jason and Dr. Todd Sala approved an addition that increased the office from 9 operatories to 27, with minimal use of square footage. In addition, we incorporated consolidated sterilization and resupply, mobile technology and supply delivery, and treatment rooms that could be immediately converted from left-handed to right-handed. Because of these changes, Sala Family Dental can now accommodate many more patients.

Many dentists who don’t learn how to scale up settle into a solo practice. It isn’t that a solo office is a great idea—in fact, it’s an impediment to a lot of the technology that has become the standard of care. But some doctors just find so much “headwind” when trying to move forward that they simply stop trying.
Benefits for Dentists
One of Dr. Barnes’s mantras is to help dentists become better and more productive. I wholeheartedly agree with that philosophy. In a very practical way, my goal is to help dentists increase production. Typical performance for a dental practitioner is about $450–$460 per hour. My goal is to increase the doctor’s productivity. It’s worth noting that this metric (production-per-hour) is critical for a variety of reasons. Production-per-hour is comparable across every dental practice. It can be normalized based on procedure prices.
The Practice Productivity Review is one of the many tools I use to gauge a practice’s efficiency. By tracking production-per-hour and other metrics, dentists gain a deeper understanding of the overall robustness of their practice. It can help dentists clarify and refine their goals for the future.

If a doctor becomes truly productive, he or she can do the same amount of dentistry they are currently doing in half the time. With the free hours, they can go to the gym or to physical therapy–or do more dentistry! Making progress is all about being able to get the work done better and faster. The more dentistry that gets done, the more lives that are changed.
Benefits for Patients
Based on our research, about one-third of all dentists report that they are not busy enough. But we’ve already established that most patients want treatment. So why the disconnect? Dentists often put up barriers, some of which may be unintended. Dentists should invest some thought and effort into how to make their dentistry acceptable for their patients.

Humans are visual creatures. When people walk into a room, they “read” that room in one tenth of a second—not in the frontal cortex of the brain (the “logic center”) but with the limbic system of the brain, which deals with emotions.
Patients read a room as safe or unsafe. If a patient reads the exam room as unsafe, then the dentist has to do a lot of extra work to get patients in a frame of mind where they can start thinking about accepting the care that they need.
Dentists often don’t understand this concept because they are accustomed to their office and don’t view it as scary. But when a patient walks into an office that has a funny smell, and he or she hears frightening sounds and sees scary equipment, it’s no wonder the patient doesn’t buy the dentistry! Luckily there are ways to accommodate this perception.
The techniques involve simplifying what a patient sees upon entry to the operatory. Removing clutter from the floor and sidewalls gives an operatory a greater sense of space. Locating the “scary” instruments out of a patient’s initial view helps prevent a “fight-or-flight” reflex. Lighting also plays a significant role–an indirect, ambient light source is critical.
A while ago, a 16-year-old young woman with discolored anterior teeth visited my practice. She had been working a part-time job and saving her money for the last three years to afford treatment for her teeth. By the time I walked in and greeted her, she had already had four or five contacts with my office.
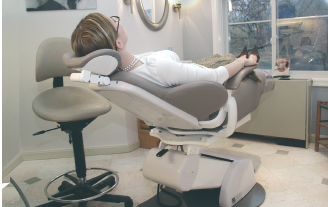
![]() Sitting in the dental chair, she looked at me and said, “I’ve been to five different offices and this place just feels right. You are going to be my dentist.” I didn’t get a chance to tell her anything about how the ceramics were going to help or how wonderful my margins were. She made her decision because it just “felt right” to her. The patient opted in for treatment because of an environment for care that created a level of emotional comfort and security.
Sitting in the dental chair, she looked at me and said, “I’ve been to five different offices and this place just feels right. You are going to be my dentist.” I didn’t get a chance to tell her anything about how the ceramics were going to help or how wonderful my margins were. She made her decision because it just “felt right” to her. The patient opted in for treatment because of an environment for care that created a level of emotional comfort and security.

Injury Prevention
As I learned early in my career, ergonomic injuries are prevalent in dentistry. A lot of dentists (and their team members) experience physical discomfort. The injuries vary with the different positions in the practice. Dental assistants tend to have a lower incidence of injury than dentists, likely because dentists usually grossly underutilize their assistants.
Hygienists have a higher incidence of injury because they are doing more repetitive activity. Assisted hygiene (with a dedicated hygiene assistant) should be done thoughtfully, because with more patients, the frequency of repetitive stress injuries can increase, too. I don’t mean that it is a bad idea; it simply has to be done correctly. There is no real reason for hygienists to have higher incidence of injury than dentists.
Certain changes can be made to address these issues. One is much higher use of ultrasonic scalers, which can significantly reduce muscle strain. Another is to alter the sequence of the hygiene appointments to increase flow.
Tips to Get Started
Doctors often tell me, “I want to just fix one room.” Rather than starting with redesigning a room, I suggest changing the way you do things. Again, analyze the overall workflow. Think about everyday tasks that are wasteful—wasteful of time, effort, and resources. Eliminate anything that is unproductive.
Initially, I almost always advise dentists to reposition the doctor and assistant. Specifically, change their position to give the assistant better access to the patient, which will improve the assistant’s performance.
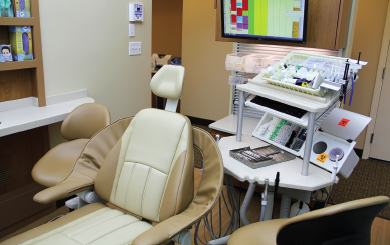
Second, get all of your supplies in close proximity. In virtually all dental practices, the assistant spends a lot of time on “go and gets” within a procedure—the assistant has to get out of the field to retrieve needed materials.
![]()
Every time a team member is not working directly on the patient’s mouth, the procedure takes longer for the patient, and it’s worse for the tooth, too. The assistant has to reach all over the place (which is another reason they use belly bars) to get supplies that are behind them, or in drawers, or somewhere else.
It’s better for the patients and for the team’s overall productivity to limit the time spent reaching for supplies, and instead spend more time on the actual treatment.
Many doctors tell me, “I’ve got so many supplies, I can’t have them all near me.” This is simply wrong—and addressing this fallacy presents a huge opportunity to improve both practice productivity and health. It’s all part of the science of deployment.
This was one of our key early discoveries, and came into focus when I began studying the Toyota Production System and LEAN manufacturing. I found out that with some forethought (and a patented design or two), we could position a full 10 days worth of all supplies and consumables within an ergonomically healthy reach of both doctor and assistant.
These supplies were stored in modular bins and tubs, and specifically prepared to accommodate our most common procedures (roughly 90 percent of dental treatments).
Supplies for less frequent procedures were kept in separate tubs and deployed as needed. The fact that these tubs leave the operatory for restocking allows for a centralized resupply area, where it is much easier to control and maintain inventories.

![]()
My Life’s Work
When I began this work over two decades ago, I was simply passing along my newfound knowledge to other dentists. Building a successful company wasn’t my intention, but something I did in my spare time.
Eventually, I built an organization around that knowledge. It was at least five years before I fully realized that I had a design company! The principles that Dr. Dick Barnes introduced me to and my subsequent discoveries have essentially become my life’s work.
For me, my dental practice is now where I go to relax. After a busy day of business meetings, it feels amazing to practice dental work. I do everything I possibly can to get to my practice every week—it’s truly my happiest time. At my practice, I help people have dream weddings, get new jobs, and restore lost self-esteem. It’s such an honor for me to do that for my patients on a weekly basis.
In addition to helping patients, I’m also a “test pilot” for new equipment and techniques. My design company is constantly innovating and looking for different ways to advance the industry. As a result, I get to create smiles for people while testing and refining the technologies and tools we develop.
Too often doctors are a bit short on the vision side of things. They miss tremendous opportunities. We have the greatest profession in the world! I don’t think enough doctors appreciate that, in part because dentistry is so stressful for them. I want every doctor to enjoy dentistry as much as I do. It can start with something as simple as changing your wardrobe or as comprehensive as changing your life. It’s up to you to start today.









