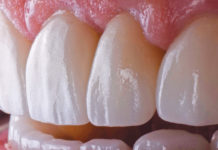
DENTISTS CAN PLAY A CRITICAL ROLE IN SLEEP APNEA DIAGNOSES.
In the previous issue of Aesthetic Dentistry (Summer 2013, Volume 12, Issue 1), I discussed the theory that in some cases, people are clenching and/or grinding their teeth (or just contracting their muscles) while they sleep in order to help maintain a patent oropharyngeal airway (what I refer to as “protective function” in contrast to the typical term of parafunction). This concept of connecting sleep apnea to certain types of bruxism has been around for years, but it has recently started to gain traction in mainstream dental continuing education.
What should you look for when screening your patients for possible sleep apnea-related bruxism, as well as other signs, symptoms and comorbidities related to obstructive sleep apnea (OSA)? Your patients present these issues every day, but you may not have seen the signs. It is amazing how blind we can be to obvious signs and symptoms, when we don’t know what to look for:
Some Dental Signs and Symptoms Correlated with OSA:
• Wear of the teeth (particularly anterior wear). This also includes chipped or fractured restorations. Wear may also include chemical erosion from gastroesophageal reflux disease/heartburn, which has a higher prevalence in patients with OSA. Wear also includes wear facets from clenching.
• Scalloping on the borders of the tongue (from thrusting the tongue against clenched teeth).
• A crowded oropharyngeal airway (large tonsils, elongated uvula, and/or elongated soft palate).
• Mandibular tori, or tori/exostoses in general. Periodontal bone loss (the opposite of mandibular tori), is starting to be correlated with OSA as well.
• Mouth breathing, particularly in children.
More than 95 percent of patients who have an in-lab sleep study are diagnosed with sleep apnea. Take a moment and visualize the typical sleep apnea patient. Did you visualize an older, heavyset male? If you did, you correctly identified the person most likely to have sleep apnea. The problem is that most physicians are only referring such patients for sleep studies. That’s messed up! Obviously, we are missing lots of people with sleep apnea who don’t look like overweight, mature men. Women and children aren’t being identified. However, in my practice and in the recent research literature, we are seeing (because we’re looking) OSA in more and more people who do not fit the stereotype.
Signs and Symptoms Correlated with Adult OSA Include:
• Snoring (but not everyone with sleep apnea snores)
• Gasping or choking while sleeping
• Non-refreshing sleep
• Fatigue or daytime sleepiness
• Poor memory
• Erectile dysfunction*
• Hypertension
• Heartburn and GERD*
• Depression (particularly in women)*
• Fibromyalgia*
• Chronic Fatigue Syndrome*
• Headaches*
• TMD issues*
• Bruxism
Signs and Symptoms Correlated with OSA in Children Include:
• ADHD/hyperactivity*
• Poor school performance*
• Developmental delay*
• Enuresis*
• Headaches*
• Earaches
• Nightmares/night terrors*
• Snoring
• Bruxism
Ask yourself: if the diagnosis is incorrect, how likely is the treatment plan to be correct?
With regards to children, based on the current literature and my personal experience, I believe that any child who snores and has evidence of bruxism should be evaluated for sleep apnea. If you think a child may have sleep apnea, it is typically better to send the child directly to a pediatric sleep specialist, rather than to an ENT physician. Even though the first line of therapy for OSA in children is removal of the tonsils and adenoids, many ENTs will not be able to treat the child without documentation of several strep throat infections, or diagnosis of OSA (with an AHI greater than 1.5).
Research shows that ADHD is correlated with OSA, and that when the tonsils are removed in children with OSA, their ADHD is often resolved. I am not suggesting that all ADHD is directly related to OSA. What I am suggesting is that before my child started taking a serious prescription medication, I’d make sure he/she had undergone an in-lab sleep study to rule out sleep apnea first.
The same principle applies for depression in women. If a woman walked into a doctor’s office and reported symptoms of fatigue and low energy, depending on the doctor, she is likely to receive a prescription for an antidepressant (which can also cause bruxism). Again, I am not suggesting that all depression is directly related to OSA. What I am suggesting is that before my wife or daughter started taking a prescription antidepressant, I’d make sure they’d undergone an in-lab sleep study to rule out sleep apnea first.
So How Can We Easily Screen Our Patients?
There are several screening forms used widely in sleep medicine (and easily found online), such as the Epworth Sleepiness Scale (ESS), the STOP-Bang and the Berlin Sleep Questionnaire. In my practice, I have created a unique screening form using the ESS, STOP-Bang questions, and a few additional questions of my own, such as:
• Name, today’s date, DOB, height, weight?
• Have you ever been diagnosed with obstructive sleep apnea (OSA)?
• Are you currently being treated for OSA?
• Are you aware of a family history of OSA?
• Are you aware of clenching or grinding your teeth at night?
I recommend that all dentists create a screening form to give to every patient that walks in the door. Using such a form can be very helpful and I have found that most general dentists will have roughly 25 to 30 percent of their patients report either having been diagnosed previously with OSA, clenching or grinding their teeth or scoring positive on the ESS and/or STOP-Bang questionnaires.
However, a paper screening form is only one tool and I rely far more on a history and evaluation with the patient than on any screening form—particularly for women. Women rarely describe themselves as being sleepy or falling asleep in certain situations (which the ESS measures). They generally describe themselves as being fatigued or tired. The STOP-Bang questions are slanted towards diagnoses of overweight men, so it won’t necessarily identify women, and certainly not children.
If you ask a woman with even a little bit of noticeable tooth wear, if she happens to snore, you will be amazed at how often you hear her respond with a slightly embarrassed, “Yes! Why do you ask?”
Once you identify a patient with possible sleep apnea, the first step is to educate the patient on what you believe you are seeing—seeing now for the first time even though they may have been your patient for 20 years! Explain to them that you care about them as a dentist and friend, and that you would like them to be evaluated by a family physician or sleep doctor.
If you’d like to immediately protect them, you might suggest something like the Silent Sleep™ appliance, or some other temporary appliance, to protect their airway and their teeth while they are going through the diagnosis process. If you decide to use the Silent Sleep™ or another temporary oral appliance, I recommend billing it out as a nightguard to dental insurance, since you are treating bruxism at this point, until you have an actual diagnosis of sleep apnea.
For most dentists, I recommend talking with your patient’s family physician about possibly referring the patient for a sleep study. This could be an in-lab or an at-home study. Talking with the patient’s family doctor helps build a rapport with the physician, helps the physician start seeing more signs and symptoms, and helps make the physician aware that you can help their other patients with snoring and sleep apnea (including those who have already given up on continuous positive airway pressure— CPAP). Once you become a little more comfortable, you may start referring patients directly to sleep doctors like I do, but I recommend starting with the family practitioners.
Please don’t make this about getting the patient back for an oral appliance! Have the integrity to care enough about a patient to give them the best treatment possible, which is the treatment that will work and that they’ll actually use. I never dictate that a patient return to me for an oral appliance. However, I do educate patients that in most cases, if their sleep apnea is diagnosed as mild or moderate, an oral appliance will most likely be an option. At that time, I show them an example of an oral appliance so that they’ll know what I’m recommending (Arrowhead Dental Lab and many others offer appliances on models for demonstrations). Then, the patient often requests an oral appliance,rather than me telling the doctor that I want them to send the patient back.
Believe it or not, treatment of sleep apnea is pretty easy, as long as you’re an expert in TMD. Well, maybe expert is too strong of a word, but the more you understand TMD issues, the more you’ll be able to recognize problems before they occur and the better you’ll be able to take care of problems when they occur such as TMJ pain, muscle pain and occlusal changes.
I’ll discuss t hat topic in depth in a future article, but if you need additional support in the TMD-area, please consider joining me on January 10–11, 2014 in Salt Lake City for the Dr. Dick Barnes Group two-day, TMD seminar. In this course, I will explain the most common types of TMJ disorders and how to deal with them. This knowledge and skill will make administering oral -appliance therapy for sleep apnea much more comfortable.
Now it’s possible to start “seeing” potential OSA in your patients. It’s there. It’s always been there. But don’t beat yourself up a bout not seeing it before. The unbelievably fantastic newsis that you now have the opportunity to participate in savin g a patient’s life! This is not hyperbole! People are dying from events directly r elated to OSA. People everywhere are suffering from the effects of OSA and poor sleep. You can literally add years to people’s lives and life to their years. How cool is that?
CLICK HERE to read Dr. Spencer’s previous article on bruxism titled “Think You Know Everything About Bruxism? Think Again!”