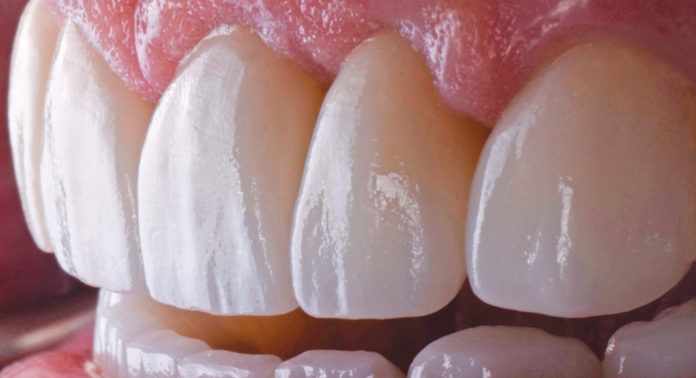
Taking the Time to Get Things Right on a Smile Makeover.
I first met Daniel in December 2017. His wife had been a patient in our practice for eight years, but we hadn’t treated Daniel. She had wanted him to come in for some time, but he’s a busy guy who owns his own company. It had been a long time since he’d visited a dentist. His teeth had been giving him problems for a while but taking care of them wasn’t a priority. Eventually, it got to the point where the timing was right and he decided to take care of his teeth.

 In the initial consultation, we discussed Daniel’s concerns and how I could help him. I asked him how his teeth had gotten into their condition. He said that he had a history of not taking care of his teeth and even abusing them somewhat—including everything from generally neglecting them to using them to open bottles and cans, and grinding them at night.
In the initial consultation, we discussed Daniel’s concerns and how I could help him. I asked him how his teeth had gotten into their condition. He said that he had a history of not taking care of his teeth and even abusing them somewhat—including everything from generally neglecting them to using them to open bottles and cans, and grinding them at night.
Now Daniel was motivated to get his teeth fixed. Initially, because his teeth were so broken down, I was considering giving him a hybrid denture or something similar, but he was not interested in that. He wanted to keep as many of his natural teeth as possible.
I considered doing some posterior implants in the molar areas of the mandible, but he had been missing teeth so long that the bone was severely atrophic. There was not enough room above the inferior alveolar nerve to comfortably place implants. He had tooth numbers 20 through 29 in the mandible, and he had tooth numbers 2 through 11 and 15 in the maxilla. But tooth numbers 2 and 15 were non-salvageable.
With the denture option off the table, I talked to Daniel about visiting a periodontist to get his gums healthy. I explained that if he wanted to keep as many teeth as possible, he would need crown-lengthening surgery. He was fine with that.
After the initial consultation, I brought him back for a comprehensive exam where we took photographs (a full mouth series of X-rays), performed a soft tissue exam, did initial charting, took impressions, made a facebow record, and took a centric relation bite utilizing a leaf gauge. Once we got his case mounted in centric, I could tell that we probably had some room to get decent-sized teeth for him.
Preparatory Work
After our initial diagnostic work, Daniel went to the periodontist. There was no way to place temporaries on his teeth in their current condition because they were so short. All I could do was refer him out to try to get some more tooth structure to work with.
I asked the surgeon to give Daniel 2 millimeters of ferrule for each tooth so that I could restore them with crowns. He did 360-degree crown lengthening on tooth numbers 6 through 11. Other areas were treated with scaling and root planing.
The periodontist had to remove two teeth that were not in function and non-restorable—tooth numbers 2 and 15. He also performed a sinus lift and placed implants in the 12 and 13 positions. Daniel also had to visit an endodontist to have root canals on tooth numbers 3 and 9.
Case Execution
It was about three months before Daniel was ready for me to start working on his restorative dentistry. My top priority was seeing how he would function in temporaries. I like doing temporaries chairside because they are not as rigid as the ones from the lab. It may seem counterintuitive, but the chairside temporaries reveal a lot of important information. I view them like the canary in the coal mine—if there’s a weak point in the occlusion, it will show in the chairside temporaries.
The case was mounted in centric relation and I sent it to Arrowhead Dental Laboratory in the greater Salt Lake City, UT, area for the White Wax-Up. When it arrived it looked beautiful. I wanted to give Daniel the appearance that he wanted along with the function he needed. Once his mouth had healed, we prepped his teeth.
At the first appointment, we prepared the maxillary arch. The next day, we prepared the mandibular arch. The temporaries were fabricated from Luxatemp and we cemented them with Temp-Bond™ Clear.
There was a minor hiccup with the temporaries. They did not line up with his preparations. So I took impressions of the preps on both arches and sent those off to Arrowhead to have new wax-ups made. In the meantime, I patched together what we had so that he would be able to function with it.
When I mounted his case, I noticed that Daniel was hitting on his premolars. Tooth number 4 touched tooth number 29 in centric relation, but the moment he applied any pressure on it or postured forward, his teeth came together in the anterior. That had been going on his entire life.
 Centric relation is a great place to start working from, especially if dentists don’t have any information to go on—as was the circumstance with this case. Initially, trying to put Daniel into centric relation wasn’t natural. I tried to give him a little bit of overjet, and it ended up being too much. He kept breaking the temporaries between tooth numbers 6, 7, and 8. He came in multiple times to have it repaired.
Centric relation is a great place to start working from, especially if dentists don’t have any information to go on—as was the circumstance with this case. Initially, trying to put Daniel into centric relation wasn’t natural. I tried to give him a little bit of overjet, and it ended up being too much. He kept breaking the temporaries between tooth numbers 6, 7, and 8. He came in multiple times to have it repaired.
Once I got the new wax-up, I made Daniel a new set of temporaries, reducing the height of the teeth, but he still kept breaking them between tooth numbers 6, 7, and 8.
I had to do some problem-solving to figure out how to prevent this from happening. I concluded that I had given him an envelope of function that was too steep, and he had adapted to a more down-and-forward posture. That’s where he was comfortable.
I re-did the temporaries, making them a little shorter and a little shallower. This gave Daniel more freedom to move, which worked out much better for him. He finally felt comfortable after this fourth attempt at the temporaries, and he didn’t experience pain or feel entrapped.
Take Your Time
Many patients think that a smile reconstruction can be a one-day process and they can get a dramatic makeover really quickly. But it pays to take your time and make sure you’re doing it right. Daniel’s case is a good example of proceeding slowly and strategically.
Acrylic temps are stiff, hard, and durable, and they are typically splinted together. If I had used such temps, Daniel might not have broken anything due to their durability. I may not have discovered the overall problem until I had switched to individual crowns.
To get things right, I had to do more than shorten the temporaries, because Daniel didn’t have freedom of movement. Again, his envelope function was too steep, and that’s why he was breaking them.
 So instead of just making them shorter, I also had to flatten or make the lingual side of the teeth shallower in order to give him better guidance. Otherwise, Daniel would have kept breaking his temporaries.
So instead of just making them shorter, I also had to flatten or make the lingual side of the teeth shallower in order to give him better guidance. Otherwise, Daniel would have kept breaking his temporaries.
I also changed his vertical dimension of occlusion (VDO) because he was over-closing. His premolars would hit, and then he would slide down and forward, and that’s why the teeth would come together in the anterior. I put him back to where he was before his front teeth got destroyed. Over time, he had various teeth taken out in different areas and was left with no posterior support, so he was always functioning on his front teeth.
Despite such issues, Daniel reported experiencing no joint pain. If he had come in with a sore jaw or if I had made temporaries and he had reported joint soreness, that would have been a different story. But there was no reduction of his ligament, no clicks, no pops, and no tears. That knowledge helped in determining the direction of the case. If he had temporomandibular joint (TMJ) issues and the temporaries had made them worse, that would’ve been extremely problematic.
Daniel was in various sets of temporaries for a total of about five months, living with them and getting a sense of how he functioned in them. He was in the final set for about a month. Those were the ones that ended up working the best and that he was in the longest without any issues. Knowing that the final temporaries were working gave me confidence that I had achieved a comfortable, functional position for him.
Once we got the right shape and size of restorations and Daniel was tolerating them, we impressed the temporaries for the final restorations. When those restorations arrived, Daniel came in and I seated both uppers and lowers in the same appointment. It took about three hours.
I chose aesthetic zirconia for the final restorations because I wanted something stronger than e.max and also more aesthetic than full strength zirconia. We used RelyX™ Ultimate for the cement and Scotchbond™ Universal as the bonding agent.
After seating, I immediately checked Daniel’s occlusion to get him comfortable and then he went home. I brought him back the next day to again adjust his occlusion. One week later, Daniel visited our office and I used a T-Scan by Tekscan® to digitally check his occlusion and protrusive movements. The T-Scan helped to make the adjustments easier. Today, Daniel uses an occlusal night guard. We see him regularly for hygiene appointments, and he seems compliant with wearing it.
 Case Outcome
Case Outcome
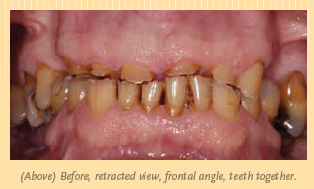
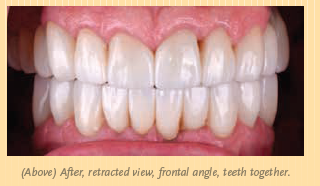
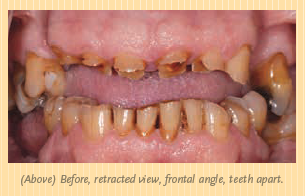
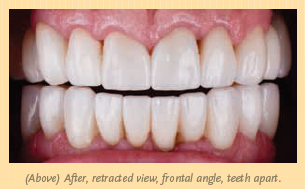
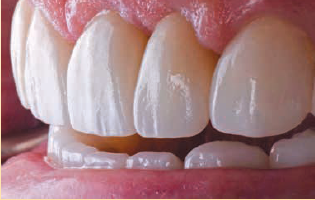
Daniel was thrilled with the results. His wife was at the seating appointment, and she was very emotional. As you can see in the photos on pages 13 and 14, it was a dramatic change. Patient happiness is always the most important outcome—and also the most rewarding.
Daniel’s case wasn’t an easy, straightforward one. There were a lot of factors to consider, including how his teeth had deteriorated, and how we could prevent the same thing from happening to the permanent restorations.
I had to proceed slowly and understand that this was not a simple case where I could prepare him, top and bottom, temporize, take a full arch impression, and then send it in and say, “Go ahead and make the permanent ones,” knowing it would work out fine. I had to take time to work things out for Daniel.
Because we worked methodically through all the issues, I didn’t have a lot of surprises with the case. The work that the periodontist did turned out great. The implants were in a good position. The endodontist did his job. Working with the different temporaries helped us get everything into the right position.
In addition to fixing the problems Daniel was having, I wanted to prevent such problems from happening again. Using zirconia restorations helped because they are so strong. But in addition to that, keeping regular hygiene appointments, alternating between the periodontist and my office to make sure there are two sets of eyes on him, wearing the occlusal guard at night (a must for him), and simply not using his teeth as a tool to open things are all important to the future success of Daniel’s new smile.

I did my best to plan in case anything were to fail. Daniel has one area where there is a bridge—tooth numbers 3 and 4 are splinted, and tooth number 5 is a pontic to 6. Everything else is an individual unit, so if one of them were to fail, he could easily have an implant placed.
I tried to make sure Daniel’s occlusion was protected and that he would be able to function well with it. I can’t predict if he is going to get decay, but as long as he keeps up his hygiene, it should be fine. Decay wasn’t really a huge issue for him in the past. His main problem was wear and tear.
What I Learned
Working on Daniel’s case has taught me the importance of taking the time to get it right. Daniel was great because he did not rush me on this case. He did not give me a deadline of when the work needed to be done.
When I said I wanted him to stay longer in the temporaries, he was fine with it. He never said, “Let’s get this done. I want to finish this.” Whatever the process was, he was “in.”
Dentists can get into trouble when a patient needs to get a case done by a certain date. If it’s a complicated case like Daniel’s, rushing can compromise the outcome.
I also learned how important it is to understand how the patient’s teeth got to their current condition. Even if a patient isn’t forthcoming with details, there are things dentists can deduce that will help the overall results.
Before Daniel, I hadn’t really worked on a case that was this badly broken down. I had done cases where it was a functional fix rather than an aesthetic fix, but nothing as severe as this case. It was a bit overwhelming at first. His was a multidisciplinary case, utilizing both a periodontist and an endodontist to achieve such outstanding results, and everybody had to work and communicate well together.
I think the case turned out so well because we took our time and made sure we got things done right. Sure, making the temporaries four times was not necessarily ideal, but it was worth following that process in order to achieve the absolute best placement.
The positive outcome was due in large part to the planning. If Daniel had refused to do crown lengthening, I could not have done this case. There just wasn’t enough tooth structure. I knew that the periodontist would give me more tooth structure, and that the patient was on board with everyone’s recommendations. It gave me a boost of confidence that helped the process along.
The timing was right for Daniel, and I’m glad that he was open to doing the process the right way, including going to all the specialists and spacing out the treatment over several months. He was able to keep most of his natural dentition in the process, and since then, he hasn’t stopped smiling.









