GETTING PATIENTS TO SAY YES TO TREATMENT.
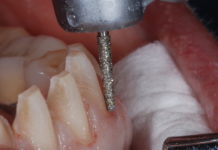
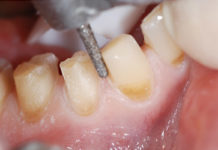
You know the drill. A patient a comes into the office after an absence of several years. After the hygienist works on the patient, he or she sees multiple issues. You do a comprehensive exam, consult with the patient, and the inevitable happens—the patient needs a full arch reconstruction. You know what you have to do, so you brace yourself; a $40,000 fee for a patient is rarely easy to present.
Does this scenario seem familiar? A lot of dentists dread presenting large-case dentistry to patients because they don’t know how to handle patient objections. But presenting large cases to patients doesn’t need to be painful for anyone—dentist or patient. Overcoming patient objections is a skill that you can work on and improve, just like any other skill.
Think about it another way. What if you don’t present large-case treatment options for your patients? Have you thought about the problems associated with not handling patient objections? Or equally as bad, modifying your treatment plan because of fear, or assuming that your plan will be rejected?
Avoiding presentation of comprehensive care can result in many problems. First and foremost, patients get less than ideal care. The repercussions of suboptimal care mean that a patient’s issues are left unresolved and usually worsen (resulting in more extensive and expensive care later on).
In addition, avoiding comprehensive case presentation limits the production capabilities of your practice. It’s fairly simple—if you don’t present comprehensively, you won’t have a chance to treat comprehensively. You’ll be relegated to small, patchwork dentistry, and your patients won’t even be aware that there might be an alternative.
Furthermore, when patients only receive basic treatment, they are less likely to recommend your practice to others. On the other hand, treating comprehensively and providing life-changing dentistry nearly always results in referrals and glowing reviews—the kind of feedback that creates a stellar reputation for you and your practice.
Case Presentation Strategy
Case presentations are part of every dentist’s job. Presenting cases effectively eliminates a lot of potential objections because patient objections are inextricably linked to case presentations.
When case presentations are difficult, it’s generally because dentists assume the worst and anticipate three main objections: money, confusion, or fear. By preparing in advance, case presentations can become much easier. The following tips will help you set the stage for effective case presentations, so you can overcome the most common patient objections.
Have a Strategy.
I’m often surprised when I ask dentists about their strategy for overcoming patient objections. A lot of dentists don’t have one! But my experience shows that thinking strategically improves the acceptance rate—sometimes by as much as 50 percent. Once you establish a strategy, you can engage in dialogue that leads to successful case acceptance.
Present the Best Dentistry Possible from the Beginning.
Some doctors utilize the following strategy: a patient comes in and the doctor doesn’t want to overwhelm him or her with too much dental work. So they just tell the patient one thing to build their trust. As a result, the doctor becomes great at doing onesie-twosie cases. Unfortunately, the patient doesn’t understand that ultimately, he or she needs more than a quick fix. Therefore, the patient never buys in to more than one small procedure at a time. Instead, you need to present comprehensively so that your patients get the best possible care from the get-go.
Show Self-Confidence.
You need to have the best self-esteem possible. This is very important. When I teach my course with the Dr. Dick Barnes Group, I ask the doctors, if you had to put a number on your forehead to represent your level of self-esteem, what would that number be (0 is zero self-esteem and 10 is optimal self-esteem)? Remember, self-confidence is a choice. You can choose to have a ten and you will exude self-confidence. I ask class members to give me a number until finally someone says, “I’m a ten!”
Why is this important? Because if you walk into a case presentation full of confidence, your patients will be more apt to listen. You’ve got to be in a place of confidence and conviction to support the pitch. A lot of younger doctors say, “Wow, I don’t know if I can tell [a patient] that big number . . . they’re going to be upset with me.” But if you backslide because you’re afraid of not being liked, you’re not helping the patient and you’re not helping yourself either.
Ask for Permission.
With my patients, I always explain that I’m going to look at everything and with their permission, I’d like to be able to tell them exactly what’s going on in their mouth. Together (with the patients), we’ll formulate a diagnosis and accompanying strategy that will help them keep their teeth for a lifetime.
Role-Play Objections with Your Staff.
Role-playing is critical and can be utilized whenever you have a new team member in your practice. For me, it started when a team member simply asked, “I encountered this objection from a patient. How should I handle it?” I decided that we would role-play the scenario in the office. Collectively, my team members offered solutions to the participants of the role-play, so they learned to overcome the objection and move the patient in the right direction.
For ideas on role-playing scenarios, write down events that staff members report to you during their daily routines. You can modify these notes later on and use the experiences for role-playing the situation in the future.
Learn from Other Industries.
Understanding human behavior is key for the adoption of new ideas in any industry. Zig Ziglar (1926–2012), an American salesman, understood the art of selling. Ziglar’s books, and those by other sales experts, offer expertise that is useful for dentistry.
Understand Patient Motivators.
Try to understand the personality style of each patient. Ask yourself, “How does the patient prefer to be treated?” Some patients prefer to know a lot of details; others prefer only knowing the “bottom line” and appreciate a direct approach. Personalities are very different, depending on their priorities.
Understanding human behavior and motivators can be helpful in overcoming objections. A popular tool for behavior assessment is the DiSC® assessment, which I find useful. ( Click here for more information about DiSC) If you know your patients’ “hot buttons,” you can schedule extra time for people who might need it to accept the value of what you present. Allow enough time to truly listen to their stories!
Ask Open-Ended Questions and Phrases.
A key to overcoming objections is to engage in dialogue with your patients, so you learn the core issues. Ask patients general questions like, “Where do you see yourself in five, ten, or twenty years from now with the health of your teeth?” I also use the phrase, “Well, tell me more about that.” The idea is to keep asking questions, like peeling back layers on an onion, to learn the real objections.
Once you have a strategy for case presentations, you’re ready to encounter your patients. As noted previously, the three main objections are money, confusion, and fear. Since you know that most patient objections will revolve around these three issues, you should be prepared for them.
The Objection Triad—Money
As Dr. Barnes says, it’s a dentist’s obligation to present patients with the finest dentistry available and help them find a way to fit it into their budget. To help patients understand financing, let’s start with the basic—who presents what.
In my office, the financial coordinator presents the finances. The dentist presents the fee—but only for large cases. If the case is small, the financial coordinator may present the fee, too. But for large cases, I always present the fee personally.
Having the dentist present a large fee is important because it communicates to the patient that this is an important issue. In addition, it allows dentists to see the reaction from the patient firsthand and immediately alleviate any questions or concerns.
Some patients are surprised by the “big number” associated with large cases, and cannot focus on anything but the total amount. For those patients, I sometimes utilize a process called fogging. Fogging is a communication technique that redirects energy and attention away from the original issue, and stops or slows the escalation of the issue.
When a patient is focused on a big number, I may respond with something as simple as, “Oh, did that surprise you?” My response gives the patient time to think about their reaction. If the patient says, “Wow, that’s a lot!” or “You guys are expensive!” I explain, “Well, just so you know, we’re not the most expensive in town, but we’re not the least expensive, either. We feel like our fees are a reflection of our above-average care.” We can’t hit all the expectations of all patients with regards to finances, but in general, we provide quality care and I believe we’ve got our fees in line.
 I always ask the patient, “Is this the type of dentistry you would like if you can work it into your budget?” Sometimes, the answer is, “No, I can’t fit it into my budget under any circumstances.” At that point, I acknowledge it and I might say, “Okay, finances are a concern for you right now.” And usually the patient will respond with why it’s a difficult time—maybe they are putting their kids through college and money is tight.
I always ask the patient, “Is this the type of dentistry you would like if you can work it into your budget?” Sometimes, the answer is, “No, I can’t fit it into my budget under any circumstances.” At that point, I acknowledge it and I might say, “Okay, finances are a concern for you right now.” And usually the patient will respond with why it’s a difficult time—maybe they are putting their kids through college and money is tight.
At that point I respond with, “Okay. Let’s do this. Let’s address the most critical area and put you on a hold status. We’ll ask you to keep coming in for your usual appointments and when your circumstances change, we’ll move on with your treatment. Does that sound fair?” It’s important to always figure out a way to keep the door open for patients to get the treatment they need in the future.
Sometimes when I ask patients if they would like to proceed with treatment, they respond with, “How much will my insurance pay?” To me, that’s a ‘yes’ to treatment. Then we can discuss the options and I introduce my financial coordinator to them so they can learn about all the available financing options. In the end, it’s simply about helping patients get the care they need.
The Objection Triad—Confusion
Another (and likely the most common) reason a patient rejects a treatment plan is because they are confused about the treatment and why it is the ideal course of action. When a patient is confused about a course of treatment, he or she may shut down and stop communicating. Helping patients understand the significance of treatment is critical to case acceptance.
If a patient’s response to a case presentation is, “My last dentist didn’t tell me that I needed all this. How come all of the sudden I need all this work?” Then you know that the patient is confused and doesn’t understand what you presented.
Education is essential in overcoming the confusion objection. As dentists, we need to educate our patients so they see the value and can understand (in the words of Dr. Dick Barnes) that the benefits outweigh the cost. Remember, it’s our obligation to present patients with the finest dentistry available and help them find out where they can fit it into their budget.
In an attempt to educate patients, however, dentists sometimes use complicated jargon that is difficult for patients to understand. As dentists, we have developed highly technical skills and the temptation is sometimes to try and explain dentistry to patients in that language. But again (as Dr. Dick Barnes says), “Don’t get too mouthy about stuff.” Speaking to patients in the language of a dentist can often lead to more frustration than understanding.
When I present treatment and I encounter a patient with body language that is defensive—arms and legs crossed, leaning back—I know that there may be a misunderstanding. At some point during the presentation, when I notice that body language, I may stop and say, “You seem a little perplexed about something.” That statement invites the patient to explain what he or she is feeling and usually opens the door to address the issues.
To avoid confusing patients, keep presentations simple, without a lot of technical jargon. For most patients, the “bottom line” is keeping their teeth for a lifetime. So how you can help them do that?
Always listen and ask open-ended questions, especially if you have a particularly reticent patient. As noted previously, the question I use a lot is, “Where do you see yourself in five, ten, fifteen, or twenty years from now with the health of your teeth?” The question opens up a lot of dialogue.
As previously suggested, consider tailoring case presentations to the personality of the patient. I recently met with a patient who is an extremely detailed person (a C personality on the DiSC® behavior model), who needs a large-case treatment that includes a fee of about $37,000. Because of my familiarity with this patient during previous office visits, I knew that he was the type of person who would ask a lot of questions about the treatment.
Based on that knowledge, I prepared a ton of information for him (nothing overly technical, though), so that he could process the material. I also knew that I would need to set aside a good amount of time for him and not rush through the process.
My scheduling coordinator made sure that I had enough time allotted for all his questions. Paying attention to the particular needs of each patient improves the likelihood of case acceptance.
Case acceptance is enhanced by visuals, too. Present treatment to patients in slide format, so you can show the patient what is needed in a sequential manner. In my office, we show patients photography of their actual teeth. We even put video clips in to illustrate the issues in their mouth.
Don’t show patients X-rays, as that can be confusing if the patient doesn’t know what they are looking at. And confused patients don’t get treatment done! If you must show X-rays, tell the patient, “I’ll be studying these to see what I can do to help you keep your teeth for a lifetime.”
After you have presented a case for your patient with all the bells and whistles (incredible before-and-after slides, etc.) at your disposal, the patient’s answer will reveal a lot about how effectively you’ve communicated the big picture.
If you get a question that begins with “Why?” then you have a patient who doesn’t fully accept what you have presented and you probably need to work on more education. If you get a response like, “I need to think about it,” then the patient probably doesn’t understand something and there are likely unanswered questions that you still need to address.
For me, it’s never about “selling” the case. It’s about being a practitioner who truly cares from the heart and wants to help patients keep their teeth for a lifetime. If you clearly present a case in a manner that patients understand, then they have little to object to.
The Objection Triad—Fear
When presented with treatment, the third main response that patients sometimes have is fear. If a patient is reluctant to proceed with treatment due to fear of pain, it is often because of a negative past experience. Again, ask open-ended questions to try and discover where the fear is rooted for the patient.
Fear-based objections can be overcome, but it requires patience and understanding. Sometimes the answer to fear-based objections is simple—giving the patient a certain amount of control may eliminate the problem altogether.
For example, I worked on a patient for years to help her with a fear-based response to dentistry. When we proceeded with treatment, I told her that if at any time she felt pain, she had the ability to stop the treatment. I explained that she could just raise her hand anytime she needed me to stop. Sometimes, during treatment, she would put her hand up and we would just give her a minute or two to breathe. It worked beautifully and she was able to get the treatment she needed.
In my practice, we always give our patients control, and that often helps overcome fear-based objections. Some patients with a fear-based objection request sedation. I don’t use sedation in my practice, but it can be an option for other patients and dentists.
As an alternative, for patients who are stymied with the fear objection, I recommend a good therapist. Therapy can help patients who may need additional expertise in the realm of cognitive behavioral therapy. That’s something beyond our skill set, so we refer that out, if necessary.
Fear is usually a result of confusion. When a patient doesn’t understand what the process is and how it will affect them, the patient is frightened of the unknown. To eliminate this issue, my team and I “preframe” the procedures for the patients. Preframing is simply telling a patient that something is going to happen before it happens. Before my patients commit to a procedure, I tell them, “Let’s talk about the day you come in and have the work done. Here’s what’s going to happen.” When I discuss in detail what the patient can expect on the day of treatment, it gives patients a sense of certainty about what to expect and eases most doubts and fears.
In general, spending time with patients (and giving them a sense of control) helps with fear-based responses and develops trust. In my office, we’ve found that if we take our time, tell the patient what’s going on, and let the patient have control if at any time they become nervous or uncomfortable, then nervous patients are reassured.
Don’t Give Up!
Improving your case presentations and overcoming patient objections is a difficult area for many dentists—but it doesn’t need to be. The three most common objections—money, confusion, and fear—can be successfully overcome through thoughtful education, a willingness to adapt to specific patient behaviors, and an eye on the goal of good dental health for a lifetime.
Most importantly, remember to show genuine caring for your patients and an honest interest in their health and well being. Every once in a while, patients are unresponsive to our attempt at helping them accept treatment. If that happens, I tell the patient, “Well, let’s do this. With your permission, we’ll check in on you once in a while and when something changes, I’d like you to keep in touch. We’ll be ready when you’re ready.”
If you consistently show your patients respect and caring, it will go a long way in overcoming their objections and move you closer to the goal of helping your patients with their dental health.