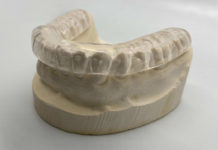
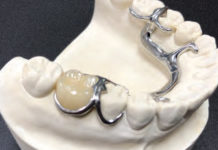
Choosing an Orthotic That Suits Your Patient’s Needs.
When it comes to orthotics, one size doesn’t fit all patients. A custom orthotic is beneficial because it is made specifically for an individual patient. With custom orthotics, dentists can choose flat or anatomical, hard acrylic or Astron (MMA-free), or even full coverage or just posterior coverage. Aesthetic Dentistry magazine recently spoke with LaMont Carpenter, Arrowhead’s Technical Consultant, about the different options and how to choose the right one for your patient.
LaMont has worked in the dental industry for more than 35 years. He is a CDT (Certified Dental Technician) examiner and is certified in four out of six dental specialties, including Crown & Bridge, Dentures, Partial Dentures, and Orthodontics.
AD: WHAT ARE THE DIFFERENT TYPES OF ORTHOTICS AND THEIR PURPOSES?
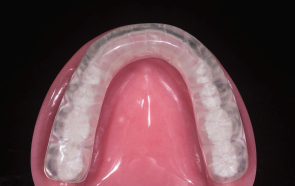
LC: A flat night guard made from hard acrylic is good for people who want something basic to protect their teeth. The Astron flat orthotic provides a good alternative for patients with certain allergies because it is made from a thermo-composite material that is MMA-free.
![]()
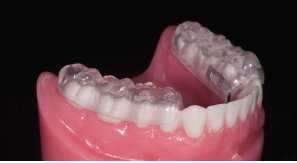
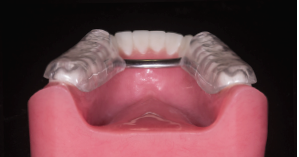
The anatomical orthotic is good because it gives the teeth someplace to rest the mandible. When a patient is grinding his or her teeth, the teeth are seeking a place to rest and the anatomical orthotic provides that place. The Gelb orthotic can do the same thing, but it only covers the posterior teeth and includes a lingual bar along the gingival and lingual surface of the anterior teeth. Patients can wear the Gelb all day and nobody will notice a thing. The Gelb appliance can be either flat or anatomical.
AD: BESIDES CUSTOMIZING AN ORTHOTIC FOR THE PATIENT’S MOUTH, WHAT CAN BE CUSTOMIZED ON AN ORTHOTIC?
LC: Orthotics can be customized thick or thin, and for the amount of coverage you want for your patients. We can also customize the jaw position. But customizing the orthotic itself for the patient’s mouth and not just having a standard size is the most important thing.
AD: ARE THERE ANY COMMON OBSTACLES YOU ENCOUNTER WHEN MAKING A CUSTOM ORTHOTIC?
LC: It’s not necessarily an obstacle, but doctors sometimes want thin orthotics for their patients because they are more comfortable in the patient’s mouth. But thin orthotics don’t last very long. If a patient is a bruxer, it’s easy to crack right through them.
A thicker orthotic will last longer. More importantly, though, the doctor should take into account where he or she wants the patient’s vertical to go. If the doctor wants to change the vertical for the patient, that’s where bites come into play and it becomes important to adjust the orthotic to where the bite should be.
![]()
AD: WHY ARE MOST DENTISTS USING ORTHOTICS FOR THEIR PATIENTS?
LC: Most dentists use orthotics to protect the patient’s teeth, new crowns, or veneers. They use them to keep patients from grinding their teeth or breaking veneers and crowns. But it’s important to remember that orthotics have additional benefits. Orthotics can be used to establish a new vertical for the patient and to help resolve the underlying issue that is causing the patient to grind their teeth in the first place.
AD: HOW DOES ONE GO ABOUT ORDERING AN ORTHOTIC TO ESTABLISH A NEW VERTICAL?
LC: The doctor will establish the new vertical they want for the patient (or the new mandibular position they want). Then, he or she will take a bite at this position, and send models or impressions into the lab. An orthotic will be made for their specific requests. Depending on the doctor’s requests and requirements, that type of orthotic will be made.
Orthotics can be very helpful for doctors trying to address issues of TMD for their patients. By changing the bite relationship in the mouth, it changes the position of the jaw joint. And that often gets patients out of the clicking and popping that they hear with TMD.
AD: DO PATIENTS USING ORTHOTICS FOR TMD HAVE TO WEAR THE ORTHOTIC ALL THE TIME?
LC: Most likely. Patients can eat and sleep and do everything in the orthotic. As I mentioned, the idea is to establish a new jaw relationship. Once patients are comfortable in a new position, the dentist can either reconstruct the mouth with a full arch or full mouth reconstruction, or do orthodontics.
The ultimate goal is to eventually get the patient out of the orthotic. After wearing an orthotic, patients will need a permanent solution. You don’t want patients living permanently with a removable orthotic. If doctors are looking at a permanent solution for a patient with TMD issues, putting the patient in an orthotic is usually the first step.
AD: WHAT DO YOU LIKE TO KNOW ABOUT THE PATIENT WHEN MAKING AN ORTHOTIC?
LC: My first question to doctors is always, “What is your goal? “Why do you want the lab to make an orthotic?” It’s helpful to know if doctors are addressing sleep issues or a TMJ problem, or what it is they are trying to accomplish with the orthotic.
An orthotic helps prevent further damage from bruxing. It helps patients to stop breaking and fracturing their teeth. But it’s important to think about what the next steps are to address the underlying problem.
AD: HOW SHOULD DENTISTS GO ABOUT ADDRESSING THE ISSUES OF FIXING THE UNDERLYING PROBLEM OFTEN TREATED BY AN ORTHOTIC?
LC: Arrowhead can help dentists customize a strategy for the underlying problems associated with a patient’s teeth. We have resources available to help dentists—whether it’s restoring the teeth to a proper position, sleep, or TMD.
Using an orthotic to help a patient is the first step toward protecting the teeth and can really be a segue or stepping stone toward having a conversation with the patient about the larger issues that are going on.
Having a conversation with a patient about extensive dentistry is not always easy. But using an orthotic is a great way to help the patient understand that this is a temporary solution to help them get out of pain and stop bruxing. Any discussion involving an orthotic should be an indication that the doctor and patient should begin to address the larger issues associated with bruxing, too.
![]()