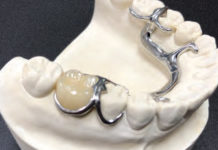
Choosing Case Materials for Optimal Outcomes.
For more than 20 years, Kent Garrick has been advising dentists on comprehensive case design. As Arrowhead’s Director of Technical Services, he recently talked with Aesthetic Dentistry about how dentists choose the materials for their cases, what the lab recommends, and tips for dentists that will ensure the materials they are using are the best choices for their patients.
AD: How should dentists choose materials for their cases?
KG: Dentists should do an overall examination to assess a patient’s occlusal situation or the bite forces before selecting materials. Dentists should consider whether they need to increase the patient’s vertical or other issues. Do they need more of a balanced group function posterior occlusion? We typically use glass throughout the arch but we craft the door stops from either porcelain-fused-to-metal (PFM) with metal occlusal or a focaled to help take some impression forces away from the all-glass restoration. Without an overall exam first, the dentist may ask for an Empress® case when they need to opt for a stronger material, such as zirconium. If patients put too much strain on an all-glass restoration, it’s doomed.
Download Arrowhead’s Material Cheatsheet Here
AD: How do prepping styles factor into material selection?
KG: Certain materials require different prepping approaches. But there’s no such thing as, “one prep fits all.” It’s easy to get into a rhythm of how to prep and sometimes doctors think it’s an all-inclusive prep. Often, doctors want Empress®, but they have left a lot of sharp edges and haven’t really softened the corners. Many dentists don’t realize that when you thin the material down to a minimal thickness at the margins, chipping and fractures happen.
AD: How does prepping for an e.max® Press compare to zirconium?
KG: With e.max® Press, you want a one-millimeter depth margin with a nice chamfer or shoulder margin. Chamfer works better than shoulder because you don’t have a 90-degree angle to get glass to adapt to. A softened edge is better than sharpened in any aspect of the preparation. We often recommend softening out corners and incisal ledges—taking a little time to round things off—because it adds to the strength and the longevity of the material.
Zirconium is a bit more forgiving, especially in terms of occlusal thickness. Because of the added strength of the zirconium, doctors have the option of an all-zirconium occlusion. It isn’t exactly like a metal occlusion, but it’s pretty close. You don’t have to stack porcelain on it. With e.max® Press, you may have exposed lithium but you still need a minimum of thickness or the case can be compromised.
AG: How do you compare that to a more traditional metal prep?
KG: Metal prep is the most forgiving because you can have sharp edges. If decay is removed from the occlusal table, doctors can fill in deeper pits and valleys with metal, because it is forgiving. At the end of the day, it’s not going to jeopardize the strength of that restoration.
AD: Should dentists always strive for the best aesthetic in every case?
KG: Often, doctors want to go with the best aesthetics, but based on the situation, sometimes there is a compromise because the patient may need materials that offer more strength. It might mean choosing a zirconium or a PFM to help stabilize the occlusion and ensure the success of the case.
AD: What kind of advice would you give a less-experienced dentist as far as the selection of materials for a full arch case?
KG: The best thing to do is to work with the laboratory from the start. Dentists should start with a diagnostic wax-up and good photographs up front. Communicating with the lab, knowing the goals for the case, and getting advice from people who work with the material day in and day out are all crucial. Every case is different and has its own unique challenges.
AD: What is the most effective and aesthetically pleasing approach to combat a dark stump?
KG: You have options, but there are compromises as well. With e.max® Press, a high opacity (HO) is available, but it may not cover as well. Zirconium has the ability to block out the dark color, but you compromise the depth of the porcelain or the aesthetics to a certain degree.
AD: How does a White Wax-up help you advise dentists on material selection?
KG: It immediately gives dentists a map of where they need to go with the case, which translates into what we can and can’t do with material. If a dentist wants to do all glass, for example, we can advise on tissue contouring or special prep requirements to get the tooth structure into the proper position for the best outcome. If a doctor wants to do all glass, we can usually tell from the wax-up if it will work or if they need a different material.
AD: What materials would you recommend when strength is the most important factor due to forces such as bruxing?
KG: A lot of problems with bruxing issues can be resolved with full zirconium. Aesthetically, that’s probably the most compromised material, but strength is more important in such cases. Out of the three options (Empress®, Zir-Max®, and PFM), full zirconium offers the least aesthetic outcome.
AD: Is there a selection that combines the strength of the metal with the beauty of the aesthetics?
KG: If you have a patient with malocclusion, it’s important to have support in the posterior, but you still have some freedom in the anterior to change that material or transition the material from a PFM or zirconium in the posterior into e.max® Press or an Empress®. I try to do that when it’s possible.
AD: What advice do you give to dentists who want to avoid making common mistakes in high-force cases?
KG: Don’t let patients dictate the direction of the case. Remember what Dr. Dick Barnes said—“Who’s the doctor, doctor?” Don’t let a patient pressure you to compromise materials in order to save a few dollars up front. Patients lack the knowledge and understanding of what may result down the road. I try to offer two options on every case, because I want doctors to feel comfortable, but I also want to make the doctor aware that there are compromises.
AD: What kind of compromises do you see that cause problems?
KG: The biggest mistakes I commonly see are under-diagnosing in general, and requesting a material that’s not going to give the best aesthetic or functional outcome. I see cases that should be a full mouth case with vertical increase, but the doctor requests to open the bite minimally or not at all. The doctor needs to look at the current wear patterns of the patient. If the anterior teeth are being worn down, but the doctor only requests work on teeth 6 through 11, there will likely be problems down the road.
AD: Are there any techniques that doctors should avoid?
KG: In an over-closed case, when a doctor only wants to do teeth 6 through 11, the doctor may try to do a metal occlusal to take care of the situation and hopefully avoid breaking glass. A lot of people don’t realize that metal on enamel will wear down the opposing teeth at an accelerated rate, so they will encounter problems down the road.
AD: What are some reasons that materials factor into case failures?
KG: Sometimes a doctor neglects to look at a patient comprehensively. All doctors should consider the longevity of the case, the happiness of the patient, and the health of the patient. Out of those three categories, one out of the three is typically considered. Treatment may need to be addressed further than anticipated by either the patient or the doctor.
AD: What material-type failures are common?
KG: A lot of times, doctors might not have the right tools or they haven’t done all the necessary research. Perhaps the patient needed more work initially—whether it was splint therapy, or vertical increase, or the proper adjustments to the opposing teeth. Maybe the doctor didn’t use a good impression material or a good tray, or was dealing with distortion. A lot of times glass is accompanied by micro-fractures. They may not show up for awhile, or the material may fail right away. When you have interferences, glass is typically the loser. Anytime you stack glass or have free-floating glass, you are set up for failure. It’s like a crack in a windshield. Eventually, something is going to influence the crack and break the whole crown.
AD: What is something that dentists do that may compromise the efficacy or strength of the material from the outset?
KG: From the start, not prepping correctly. The doctor may miss the proper reduction that the lab needs for the thickness. Sometimes, doctors say, “I was able to put a temporary on that [tooth],” but a temporary doesn’t require the same reduction as glass.
Creating micro-fractures is another common problem. If a doctor makes adjustments with burs that create heat, it creates micro-fractures. If the sequence of bonding the case is off, creating a situation with thin spots, that’s going to compromise the case. If the patient wants to make changes after a case is in the mouth and bonded, it can cause micro-fractures. If a doctor uses the wrong tools to make those adjustments, he or she will create a problem.
AD: Are there preferred ways of cementing or bonding certain materials?
KG: In the bonding process, if you tack a crown in as you’re placing it and then do a final cure, you allow yourself some damage control if needed. When you do a full cure with a crown, you’re locked in (on larger cases). With onesies and twosies, it’s pretty straightforward—make sure the occlusion and contacts are where they need to be and then just go ahead and cure it into place.
AD:Is there a strategy to remember the elements of material selection?
KG: We teach doctors to be smart about the selection in the first place. You need to know that the megapascals of each material is different and determine how you’re going to take some of the force off. We teach that putting full gold on the second as a door stop can and will minimize the compression strength or the compression forces.
I teach my tech support team that they don’t need to reinvent the wheel with every case. There are times when you need to mix and match some materials, but if you do the process the way that we recommend, you don’t need to rethink it every time. If dentists make room for the material, they want the aesthetics, and they’ve got the occlusal scheme worked out, then it’s not difficult to stick with what works.