The Dentist as Patient and the Patient as Dentist.
Dr. Ashley Blattner, D.D.S.
Our situation was unique because we started case-planning before I met the patient (Dr. Michael B. Beeler) in person! Like myself, the patient is a dentist who had legitimate concerns about his dentition and genuinely wanted to improve his smile. After talking with him on the phone, I knew Dr. Beeler would be great to work with on a full arch rehabilitation case.
The Dentist Experience
Day One (First Weekend): On the first day, I was the doctor. Dr. Beeler’s case was fairly straightforward. He presented no health concerns, and was comfortable with the prospect of extensive dental work. He wanted to fill his buccal corridor and improve the overall appearance—including shape, shade, and zenith—of his existing teeth and restorations.
After reviewing his models, we decided that improving his buccal corridor would require restoration of the entire upper arch. Dr. Beeler also had several gold onlays/inlays in the posterior that needed to be replaced due to wear, decay, and appearance.
Dr. Beeler was not a typical wear case. His Shimbashi was 16 mm, which complimented his face well. We needed to improve on his zenith, and planned for the goal of a tissue-adjusted Shimbashi of 17 mm. The treatment plan consisted of a maxillary full arch reconstruction and future lower arch reconstruction. A wax-up was completed.
Case Preparation and Execution
For prep day, I reviewed Dr. Beeler’s wax-up and checked to make sure we had the proper Shimbashi measurements. I also checked the contour and smile design to make sure it was what the patient desired. I made certain that we had a prep guide, bite registration, and stent. Arrowhead Dental Lab and Dr. Downs were great in coordinating the entire treatment and making sure these items were in place on prep day.
I was amazed by how smoothly everything went with the prep guide, bite registration, and stent. I was as conservative as possible with the prep design. I was able to stop the margin on the pre-molars on the occlusal surface, and therefore preserve the entire lingual cusp. When removing the gold onlays, I encountered some decay, but was able to excavate it and restore the areas without difficulty.
As I moved into prepping the maxillary anterior, I removed the permanent existing crowns, and soon realized that there was more tooth structure present on tooth number 7 than initially thought. We made Dr. Beeler aware of this, but we decided to move forward with a full coverage crown on this tooth (see “Challenges of Dr. Beeler’s Case” on page 19).
Once the preps were completed, I completed his temporary crowns. I was amazed at how easy the Sil-Tech® stent (made from the wax-up), was to fabricate from the temporary restorations. Not to mention how amazing they looked!
The Patient Experience
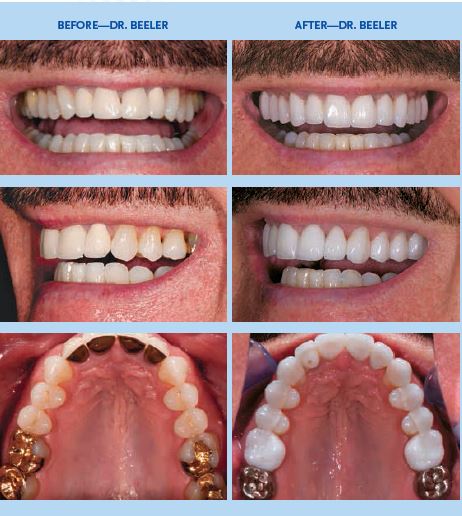
Day Two (First Weekend): On the second day of the first weekend, it was my turn to be the patient. I had decided to get my teeth done both for the professional experience and because I really wanted to change my smile. I’d had a lot of wear, but if you look at my “before” smile (see page 16), it wasn’t awful. I also had some composites and a lot of wear on my posterior teeth.
I had previously attended one of Arrowhead’s Over the Shoulder™ courses where Dr. Downs had rehabbed a young guy—he was a medical student. I looked at his mouth and thought, ‘Oh my goodness. My mouth looks a lot like his!’
So I started thinking about getting my work done. I knew I needed some posterior crown work and I thought, ‘If I’m ever going to do this, now is the time—before I need those crowns.’ I knew at my age, if I didn’t do something, in 20 years I would definitely have issues as far as posterior wear and possibly teeth chipping. I was already having some headaches, and I was clenching and grinding in the evenings and overnight.
On day two, being a patient was somewhat complicated due to the fact that I was four months pregnant. But the only real complication was with the anesthesia—it wore off really quickly. Plus, it was just tiring for me! I think I was in the chair for nine hours! I learned that it was really important to take breaks. Also, just hearing the drilling can sometimes be a bit nerve-racking.
But it was great to hear positive reinforcement while I was in the chair. During the treatment, everyone was really positive—the doctors, the lab, the technicians, and Dr. Beeler. It really helped me get through it.
Challenges of Dr. Beeler’s Case
Day One (Second Weekend): Bonding day was exciting, yet stressful. It was imperative that everything was lined up and ready to go. Dr. Beeler’s case looked fantastic—I was beyond impressed with the Elite porcelain crowns fabricated by Arrowhead Dental Lab. The quality and artistic ability that went into each one was unmatched.
We removed Dr. Beeler’s temporary crowns fairly effortlessly, except for one issue with tooth number 7. When we removed this piece of the temporary acrylic material, the tooth had broken at the gumline.
Inside, my heart skipped a beat, but I knew calmness was key, and it was nothing that the Arrowhead instructors (or any general dentist, for that matter) had not encountered before. Again, I was extremely glad that we pre-framed the possibility of such an occurrence to the patient at his prep appointment.
We continued cementing the entire arch and waited until the end to address the issue of tooth number 7. It was apparent that the tooth had a poor prognosis and would likely be best treated with an extraction and implant placement in the future.
In the meantime, we needed a tooth! We were able to fit a post into the tooth and retrofit the crown. It is not likely this will last a great length of time, but it allowed the patient to see the final aesthetic product and it bought us enough time to get an implant consult.
Reflections
It was a long day, not only for myself as the clinician, but also for Dr. Beeler as the patient. He was an ideal patient, and I gained great insight on the amount of time it takes to achieve an excellent outcome.
From the experience, as a clinician and a patient, I am now able to better prepare my own patients for what they may encounter with a full arch reconstruction. “Pre-framing” patients and telling them what they may expect is key. And what better way to do this than to tell them that you have been through the same process yourself?
The experience also taught me the importance of compassion. I have always prided myself on putting my patient first, but I really had no idea what it felt like to sit in a chair for nine hours with my mouth propped open and having my entire maxillary dentition drilled on. It is emotionally and physically draining.
Therefore, as the dentist, it is important to keep the patient excited and focused on the end result. Patients can sense a doctor’s frustration. I discovered that little breaks lightened the mood and gave the patient time to regroup. Positivity is truly contagious—it is important the entire dental team is on board with creating a fun, relaxing environment.
All in all this experience was exceptional! As both patient and clinician, the insight I gained was second to none. I love my new smile, and believe it was the best practice-builder I have done thus far. It has already opened conversations and opportunities with patients to improve their own smiles. Wear cases are difficult and a bit intimidating, but with a great lab and the confidence that comes with restoring full mouth reconstruction cases, they can actually be fun and so rewarding! The only regret I have about the process is that I did not do it sooner.